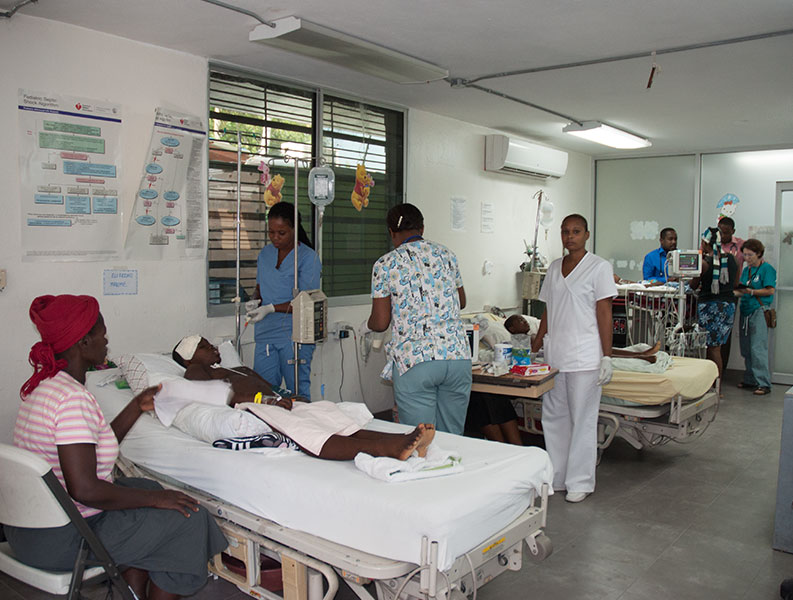
The University of Miami and Project Medishare are providing much-needed medical services to Haiti and training the pioneers of the country’s future health care workforce.

Haiti has committed $5 million to build a national trauma, critical care, and rehabilitation center, shown in this rendering.
When strolling the streets of Port-au-Prince, Wilfrid Macena likes to wear shorts to show off his right leg. With its hydraulic knee, shock absorbers, and titanium rod, he nimbly strides over potholes, dodges motorcycles, and sidesteps a sea of vendors carrying everything from eggs to couches on their heads.
“I want people to see disability doesn’t stop me,” says the former welder who received his first prosthesis at the University of Miami/Project Medishare field hospital that rose like a beacon of hope in the sea of misery left by the January 2010 earthquake.
Five years after that apocalyptic disaster, Macena, whose leg was crushed by a tumbling wall, stands as a symbol of UM’s commitment to empowering Haitians to care for their own. Now a prosthetics technician at Hospital Bernard Mevs Project Medishare, he is part of the fledgling Haitian health care workforce destined to carry out the vision of the Miller School of Medicine’s Barth A. Green. The chair of the Department of Neurological Surgery and co-founder of Project Medishare who launched UM’s unprecedented emergency response in Haiti five years ago is closing in on his dream of establishing a critical care and trauma network in a country that didn’t even have an ambulance service before the earthquake.
We were there 20 years before the earthquake and we will be there 20 years after.
Still on the drawing board but approaching reality is the $40 million critical care, trauma, and education and training center Green envisions for donated land near the Port-au-Prince airport—not far from the spot where 5,000 volunteers at UM/Project Medishare’s field hospital treated more than 30,000 earthquake survivors under four, large white tents. In October 2014 the Haitian government committed $5 million to the national center that is designed to rival UM/Jackson’s Ryder Trauma Center. Now, Green is counting on the seed money and the donated land to attract matching funds from private and international donors, whose financial help is vital for empowering Haitians to take charge of their own futures, and that of their nation’s.
And that is where UM continues to shine.
Rather than “just stirring up the dust without planting any seeds,” as Green notes many nongovernment organizations did in Haiti after the earthquake, UM faculty, staff, and students continue to help Haitians build the infrastructure and create the capacity to take care of themselves—the very reason Green and Arthur Fournier, the now-retired vice chair of the Miller School’s Department of Family Medicine and Community Health, founded Project Medishare for Haiti more than 20 years ago.
On Haiti’s northern coast, in historic Cap-Haïtien, the department’s Michel Dodard and Andre Vulcain continue to supervise and raise funds to train family medicine physicians, a specialty that did not exist in Haiti when they launched their Haiti Project in 1999. Fifteen years later, the Haiti Project has graduated more than 50 family medicine residents and generated other training programs and clinical services. Among them: the Family Practice Center, which provides a medical home to more than 30,000 patients, and an extensive HIV/AIDS service that cares for more than 3,500.
On Haiti’s rural Central Plateau, Project Medishare-trained health care advocates and volunteers from UM and beyond continue to provide comprehensive birth-to-death health care to more than 100,000 of the poorest of Haiti’s poor. Their successes are noteworthy: Infant immunization rates have climbed from less than 10 percent to 86 percent, and pregnant women now average three prenatal health care visits before giving birth. They once had none.
Yet, with inadequate water, sanitation, and nutrition a fact of life in Haiti, too many children still die young, and hundreds are born each year with hydrocephalous, an excessive accumulation of fluid around the brain. The luckiest of them undergo surgery at Bernard Mevs, the small community hospital that transitioned into Haiti’s first critical care, trauma, and rehabilitation center when UM/Project Medishare’s field hospital closed six months after the quake.
Initially run by foreign health care volunteers, Bernard Mevs is now staffed almost entirely by Haitians—the pioneers of Haiti’s trauma, critical care, and rehabilitation workforce. Bound by their own pain but propelled by new purpose, they are mentored by UM faculty and staff who continue to guide and grapple for support for the pediatrics, rehabilitation, wound care, ophthalmology, pathology, and other programs they helped launch at Bernard Mevs.
In all, Bernard Mevs’ staff treats about 100,000 trauma, critical care, and rehabilitation patients a year. Add to that number those being served with unprecedented health care in the Central Plateau and Cap-Haïtien, and UM/Project Medishare’s impact is widespread and incalculable. But it is a mere drop in the proverbial bucket of a nation of 10 million people with so much need, because, as Green notes, it takes time, perseverance, and long-term, unwavering commitment to build capacity and create sustainable health care infrastructure in Haiti.
“We were there 20 years before the earthquake and we will be there 20 years after,” Green says. “I am very proud of what we and our partners have accomplished, but it truly represents only the beginning. All that Haiti needs and wants is opportunity.”