A burgeoning pediatrics residency program is helping grow the number of doctors who can care for children in Haiti suffering from critical illnesses and disease.
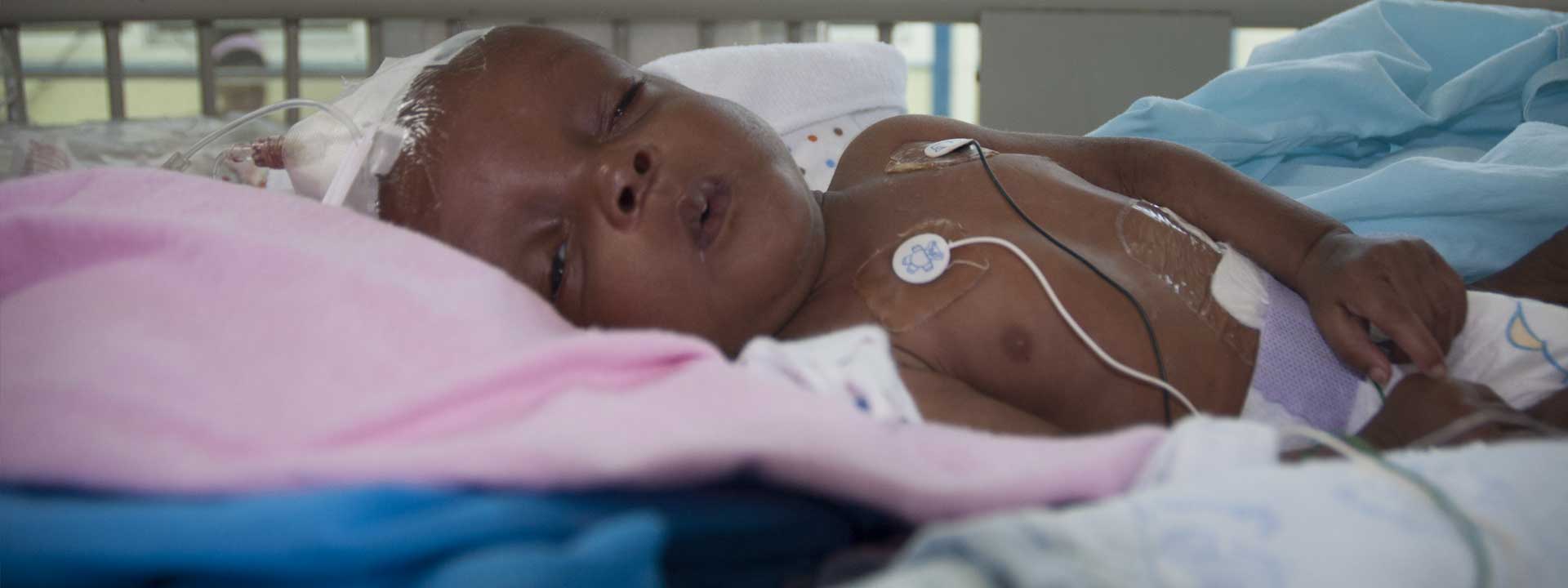
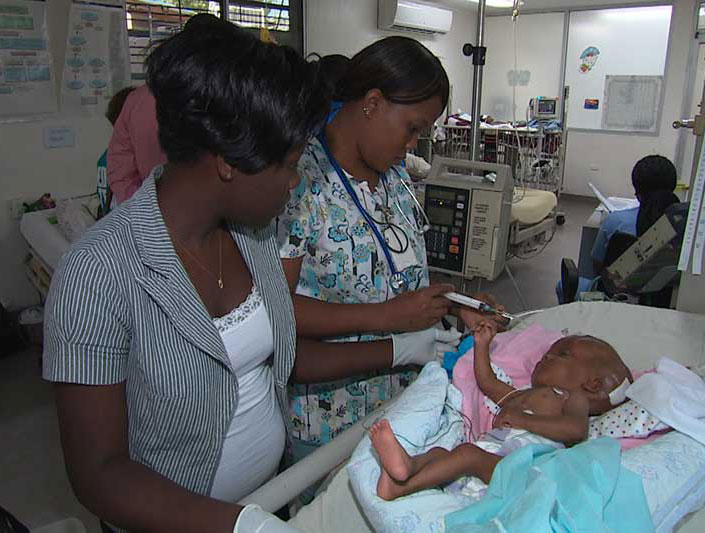
On a Tuesday morning, Miller School of Medicine faculty Antonia “Toni” Eyssallenne pays an unexpected visit to the pediatric intensive care unit at Hospital Bernard Mevs Project Medishare and is elated by what she sees. Gathered around a baby girl born with hydrocephalus, a second-year resident is briefing the infant’s mother and two attending physicians on the baby’s recovery from surgery to relieve the buildup of fluid on the brain that dooms too many Haitian newborns to death or a lifetime of disability.

UM pediatrician Antonia “Toni” Eyssallenne.
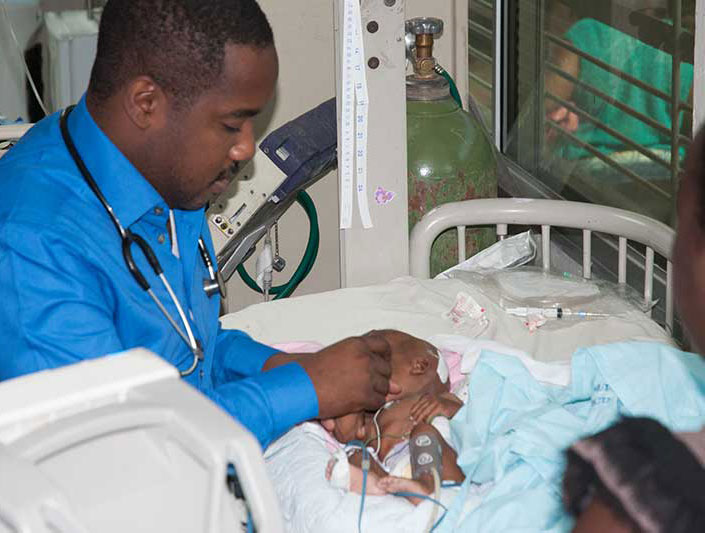
Slowly the physicians make their way around the four-bed ICU, stopping at the beds of two sick boys to talk with their worried moms. They never consult Eyssallenne, who established the pediatric residency program just over a year ago while serving as Bernard Mevs’ chief medical officer. But she is not offended; she is beaming with pride.
“I can’t believe this is happening,” says Eyssallenne, a first-generation Haitian-American who was among UM’s initial responders to Haiti’s devastating 2010 earthquake. “They are rounding with the mom. They are including her in the discussion. Engaging families is critical to improving care.”
Such scenes would be routine at UM/Jackson Memorial Hospital, where Eyssallenne completed her internal medicine and pediatrics training and now serves as associate program director of the UM/Jackson Internal Medicine-Pediatrics Residency Program at Holtz Children’s Hospital. But like the pediatrics residency program, family-centered rounding is a new concept at Bernard Mevs, which began partnering with Project Medishare 20 years ago, providing a place for UM and other volunteer surgeons to operate on children with hydrocephalus and cleft palates. Six months after the earthquake, it merged with UM/Project Medishare’s field hospital to become Haiti’s first critical care, trauma, and rehabilitation center.
Today, the 50-bed hospital and outpatient center is staffed almost entirely by Haitians who make the most of the training and unprecedented but limited resources Project Medishare and other donors provide. But when Eyssallenne, fresh from completing her four-year residency at Jackson, assumed the reins as chief medical officer in September 2010, the staff consisted almost entirely of volunteer doctors and nurses from Miami and beyond.
“We didn’t have many local human resources, and the volunteers changed on a weekly basis. It was chaotic, and very difficult to manage,” she recalls. “There were departments to structure, systems and policies to establish, protocols to adopt.”
The level of care they and their residents manage under difficult limitations is very impressive.
Particularly challenging was the shortage of pediatricians who could care for the newborns, babies, and children who arrived at Bernard Mevs in need of trauma, emergency, and critical care. While Eyssallenne could turn to UM colleagues and Medishare volunteers to fill in and train doctors and nurses in other departments, it usually fell to her to staff the pediatrics wards, which included the first pediatric and neonatal intensive care units in the country.
She soon bore the weight of Haiti’s critical physician shortage and the lack of training programs on her slim shoulders. There are only 2.6 physicians for every 10,000 people in Haiti and even fewer pediatricians—only 400 in a nation of 4 million children. Yet, there were only three pediatric residency programs with a total of 27 positions in the entire country. So Eyssallenne took on another daunting challenge.
Adapting the curriculum from UM/Jackson’s residency program and partnering with the medical school at Haiti’s Notre Dame University, she sought and won government approval to establish a joint residency program at Bernard Mevs and Hospital St. Damian, Haiti’s only freestanding comprehensive pediatric hospital.
Today, Dr. Christmen Clerveaux and 13 other Haitian medical school graduates—the pioneers of the residency program—rotate between the two hospitals, learning to care for children with cancer, sickle cell, tuberculosis, kidney diseases, AIDS, and other infectious and chronic diseases at St. Damian, and children in need of critical and emergency care at Bernard Mevs, which also includes a novel addition.
Once a week, UM’s Ilene Sosenko, the director of the neonatology fellowship program at Jackson, consults by Skype or phone with the hospital’s staff pediatricians about difficult cases in the neonatology ICU. She says she always hangs up from the calls impressed with how much they do without the diagnostic tools and other resources taken for granted in the United States.
“Even something as simple as blood tests that we order every day, or even twice a day, they can order maybe once a week,” Sosenko said. “The level of care they and their residents manage under difficult limitations is very impressive.”
The hours are long and the work is stressful, but Clerveaux is grateful for the opportunity to realize her lifelong dream of becoming a pediatrician in Haiti.
We are a poor country so we don’t have the same resources, but we have the same training as residents in Miami and I am very proud to be part of that.
“It was a tradition in our family. My mother’s kitchen was always open and our home was always welcoming to any child who needed help, so I always wanted to be a pediatrician,” she said. “We are a poor country so we don’t have the same resources, but we have the same training as residents in Miami and I am very proud to be part of that.”
Raised in New York, Eyssallenne always had her own dream of helping Haitians close the gaping holes in their health care system. That dreadful January day in 2010 when the Western Hemisphere’s deadliest earthquake left her parents’ homeland in ruins, she was about to leave on another medical mission trip to Haiti’s north coast, where she was working on a family planning project.
Instead, 36 hours later, she joined the small contingent of trauma specialists who, led by UM neurosurgeon Barth Green, Project Medishare’s co-founder, had landed in Port-au-Prince the day before and were treating scores of survivors who had been brought to a pair of cargo tents at the edge of the international airport.
She would remain in Haiti nearly a month, helping set up a triage system when the makeshift emergency clinic moved from the cargo hangers into the 240-bed tent hospital that had risen virtually overnight. The devastation and needs were overwhelming but, like the handful of volunteers who came before her and the thousands who came after, she did what she could with what little she had.
The experience would help prepare her to return to Haiti when she completed her own residency to serve as Bernard Mevs’ chief medical officer, a post she held while still working at Jackson for nearly four years—until she became director of the pediatric residency program at Bernard Mevs/St. Damian.
“Having 2.6 doctors for every 10,000 Haitians is a ridiculous number,” she says, “and adding 14 pediatricians in a nation of 4 million children is hardly enough. But we are doing what we can to fill the gap.”